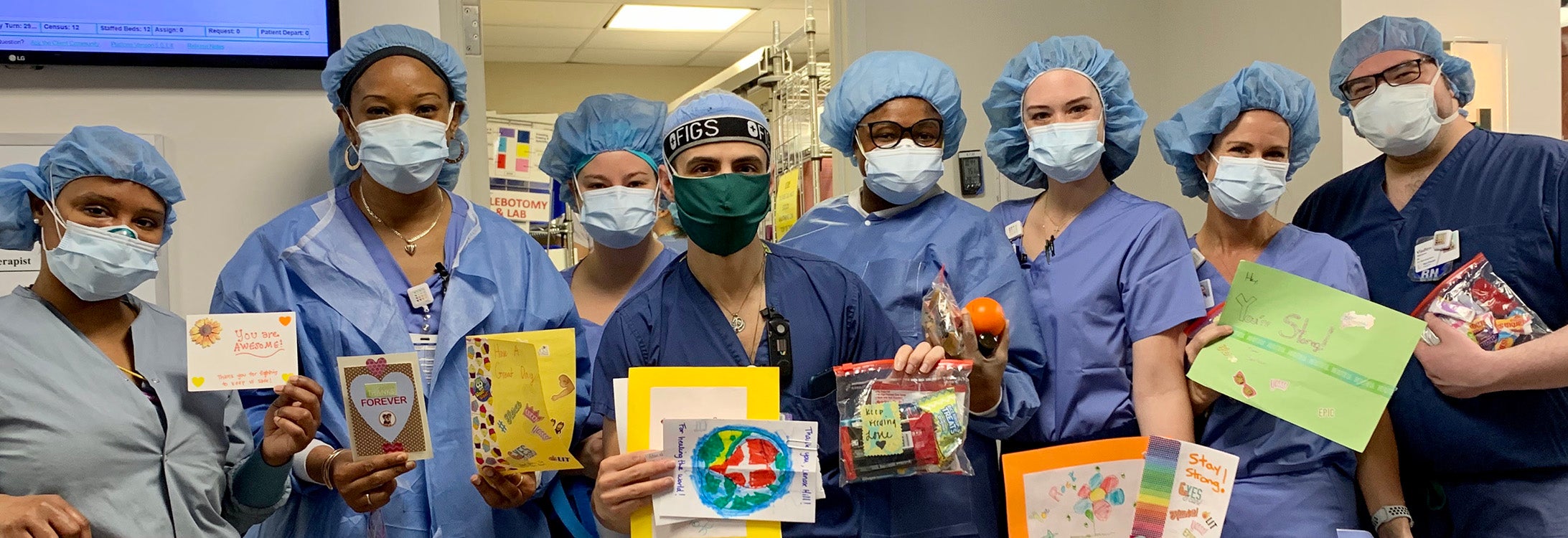
‘WE ARE FIGHTING’
ECU doctors, nurses and health care workers share stories from coronavirus front lines
East Carolina University doctors, nurses and health care workers near and far are risking their lives to serve others during the coronavirus pandemic.
From a nursing student working long shifts at an intensive care unit in Manhattan to a nursing home administrator caring for the elderly who are most at risk, these Pirates demonstrate sacrifice and resilience. They’re risking their own health — and their families’ — for the greater good. One Brody School of Medicine alumnus caring for potential COVID-19 patients worries about bringing the virus home to his newborn son. Another battles confusion over testing at his hospital in Catawba County. Here’s what makes them do what they do.
Responses have been edited for length and clarity.
JULIA LAND BATTS
From: Wilson
Graduation year: 2014, multidisciplinary studies; 2017, Master of Public Health
Occupation: Nursing home administrator at Brian Center Health & Rehabilitation/Goldsboro

Julia Batts, a nursing home administrator in Goldsboro
How has the coronavirus outbreak affected you?
The most at risk population for Americans in this pandemic are the elderly. The deadliest hot spots of the COVID-19 virus in the United States are nursing homes. As the leader of a nursing and rehabilitation facility, preparedness has been my focus. This means providing the tools, resources and support that are necessary and critical to protect our residents and staff.
What is the most intense experience you have had fighting Covid-19?
My most intense experience at this point is constantly mitigating the fear of this novel virus and the stereotypes of nursing homes that people may have. Our county currently has an outbreak in one nursing home and many individuals within the community are panicked.
What sacrifices have you had to make to do your job?
We are sacrificing our time at home and exposure to our families and community to provide the safest environment for the most vulnerable population — the elderly. The battles within nursing homes during this pandemic are much different than any other health care setting. Visitor restrictions in our industry began more than a month ago and before any other provider in the healthcare sector. We are fighting to protect our residents from the outside world. We are fighting against depression and loneliness. We are fighting boredom and confusion caused by dementia. We are fighting frustration of family members not being able to visit and families who feel disconnected and fear for their loved ones. My goal is to always establish faith, confidence, and trust in our systems, processes, and delivery of care to all individuals who are interacting with our center.
DR. BILLY PRICE JR.
From: Conover
Graduation year: 1990, M.D., Brody School of Medicine
Occupation: Medical director for Catawba County Public Health, internist and managing partner for WCA Enterprises
How has the coronavirus outbreak affected you?
As the health department physician, I have been on the front end of our community’s preparedness. I send out regular updates on our county. I continue to see patients in my office while wearing personal protective gear (PPE) and have selectively screened folks who are particularly at risk. Our COVID-19 numbers today have jumped from 6 to 35. We have unfortunately experienced a death.
What is the most intense experience you have had fighting Covid-19?
My most harrowing experience has been a total lack of coordination with a physician-led group who performed testing without proper notification. An elderly woman was tested for COVID-19 before being admitted to our hospital. She was there for two days before her test came in positive from a lab in Memphis. No one knew about the testing and it caused complete havoc at our hospital because 124 employees were exposed. She was quickly isolated.
Anything else you want to add?
I am a proud Pirate doctor!

Dr. Billy Price Jr., medical director for Catawba County Public Health
DR. SAM DAIL
From: New Bern
Graduation year: 2015, M.D., Brody School of Medicine
Occupation: Family practice and urgent care doctor at New Bern Family Practice

Dr. Samuel Dail with his newborn son, Crayton
How has the coronavirus outbreak affected you?
Our work schedule has changed greatly. Previously, I saw all of my primary care patients in person and had a very busy urgent care schedule. Now, the vast majority of my primary care visits are virtual or over the phone, which is a big challenge for many of our older patients that are not technologically savvy. The urgent care is less busy, and I think that is because people are scared to come out and potentially be exposed. Most people that are coming in now are more sick than normal and have waited longer to have problems assessed.
What is the most intense experience you have had fighting Covid-19?
Even though we are a community practice without acute care, we have still seen numerous cases of COVID-19, even people that are essentially asymptomatic. One particular patient came in with abnormal vitals and a completely unrelated chief complaint. Our goal is to make sure we can continue to care for everyone while keeping patients and employees safe. We’ve had near daily meetings to make sure our response is appropriate both for our patients and staff.
What sacrifices have you had to make to do your job?
I have an 8-week-old son that was born six weeks early. I’m always worried about being an asymptomatic carrier and exposing my wife and son. Should I develop symptoms, it would be necessary to self-quarantine for two weeks. This would be a huge sacrifice to me since he is growing up so fast.
Professionally, we are working outside of our comfort zones and really trying our best to care for our patients. The virtual visits and phone visits have major limitations. I’m very concerned about patients with multiple chronic conditions being exposed to coronavirus, but also very concerned about repercussions in three to six months if we aren’t staying on top of their chronic diseases like we normally would.
LAUREN URBAN
From: Clemmons
Graduation year: Expected 2022, College of Nursing clinical nurse specialist graduate program
Occupation: Nurse at Lenox Hill Hospital in Manhattan
How has the coronavirus outbreak affected you?
I have been a travel nurse for over two years now. I was on assignment at Emory University Hospital Midtown in Atlanta when COVID-19 first started to impact the U.S. When the health care workers on the front line in New York City were detailing their struggles with lack of PPE and personnel on the news, I reflected on the reason I chose to become a nurse: to serve others. So, I had a decision to make: Was I going to take time off away from the bedside to protect my own health, or was I going to use my skills, knowledge and able body to not only help COVID patients, but also my colleagues? I chose the latter. I was worried about taking an assignment in New York City working four to six shifts a week while also being a part-time student, but my ECU professors have provided me with constant support and understanding during this time.
What is working in a hospital in a virus hot spot like?
The morale on the units is extremely low as most health care professionals are working outside of their specialties and comfort zones. The hospital plays a clip of the song, “Here Comes the Sun” over the intercom every time a COVID patient comes off the ventilator, so it is a reminder to us that there is hope in an environment where hope can escape you easily. Focusing on the positives like this keeps me fueled to continue pushing on and uplifting my teammates as we all face this pandemic head on.

Lauren Urban (third from right), a nurse in the COVID-19 intensive care unit at Lenox Hill Hospital in Manhattan
What is the most intense experience you have had fighting Covid-19?
On my first day at Lenox Hill, we were supposed to have classroom orientation. Instead, we were rushed to get badges made so we could help with an emergency. The pressure in the hospital’s oxygen delivery system dropped. Since most COVID patients are severely hypoxic and require high levels of oxygen, hospital workers had to rush to manually deliver oxygen to all patients on ventilators. At the time, we didn’t know how long we wouldn’t have a reliable oxygen supply, so it was chaotic and frightening to hear all of the alarms and see patients becoming unstable. The issue was eventually resolved and there is now an oxygen truck outside the hospital giving us a supplemental supply.
NATE CREECH
From: Wendell
Graduation year: 2010 BS, Biology; 2012 Master of Public Health
Occupation: Emergency management team leader at WakeMed Health & Hospitals

Nate Creech, emergency management team leader at WakeMed Health & Hospitals
How has the coronavirus outbreak affected you?
The WakeMed Hospital Emergency Operations Center opened staffed on March 12 and initiated our response to COVID-19. Since the initial notification in January, our team, along with multiple other departments and personnel, has been available 24/7 for system support.
Daily activities and operations have changed completely. Organizing, leading, and attending daily briefings, conference calls, and meetings for our Operations, Task Forces, and Incident Management Team have filled my calendar. Planning and providing system-wide updates are daily tasks, including weekends, which have led to many long days and nights.
What is the most intense experience you have had fighting Covid-19?
The most intense experience I have had during this incident is working with our management team and multiple task forces to provide guidance based on the constantly evolving recommendations and guidelines. Plans, policies and procedures that would normally require months of preparedness were being developed and implemented within hours or days with the support of every single department within the hospital. Seeing this process evolve was intense, but amazing. I have had the opportunity to collaborate with some of the best nurses, physicians, staff and administration around. Seeing the teamwork and support for everyone has truly helped and been inspiring.
What sacrifices have you had to make to do your job?
The work-life balance has been difficult to manage. Long hours spent at work during the week and weekend lead to short hours at home. It has taken time to adjust to the new schedule and find time to get things accomplished outside of work.
COLLEEN CARBOY
From: Dallas, Texas
Graduation year: 1986, College of Nursing
Occupation: Nurse at Englewood Hospital in Englewood, New Jersey
How has the coronavirus outbreak affected you?
I returned to nursing after more than 25 years working as a trial lawyer after hearing about the serious shortage of nurses in New York and New Jersey on the news. After I heard that patients in Italy were dying due to the shortage of healthcare providers, I knew it was something that I just had to do. Even though I am only three weeks into my assignment as a COVID-19 crisis nurse, I know that I am making a difference. The technology being used in hospitals has changed a lot over the last couple of decades, but my nurse colleagues have been incredibly supportive and helpful. This experience has been humbling but incredibly fulfilling at the same time. I was fortunate to have a skill that could make a difference when it really counts.
What sacrifices have you had to make to do your job?
When the pandemic hit the U.S., I updated my will, gave my family long hugs and joined a COVID-19 unit at a hospital in northern New Jersey. Our unit used to be day surgery, but we turned it into an isolation ward with two beds crammed into single patient rooms. The nurses rarely take any breaks. The patients are very sick and resources are thin. We stay strong and positive because our patients need that right now. Our hospital sent its 500th COVID-19 survivor patient home recently! The nonessential staff went to the lobby to give the patient a big cheer. It was a great way to celebrate.
Colleen Carboy returned to nursing after more than 25 years working as a trial lawyer after hearing about the serious shortage of nurses in New York and New Jersey.