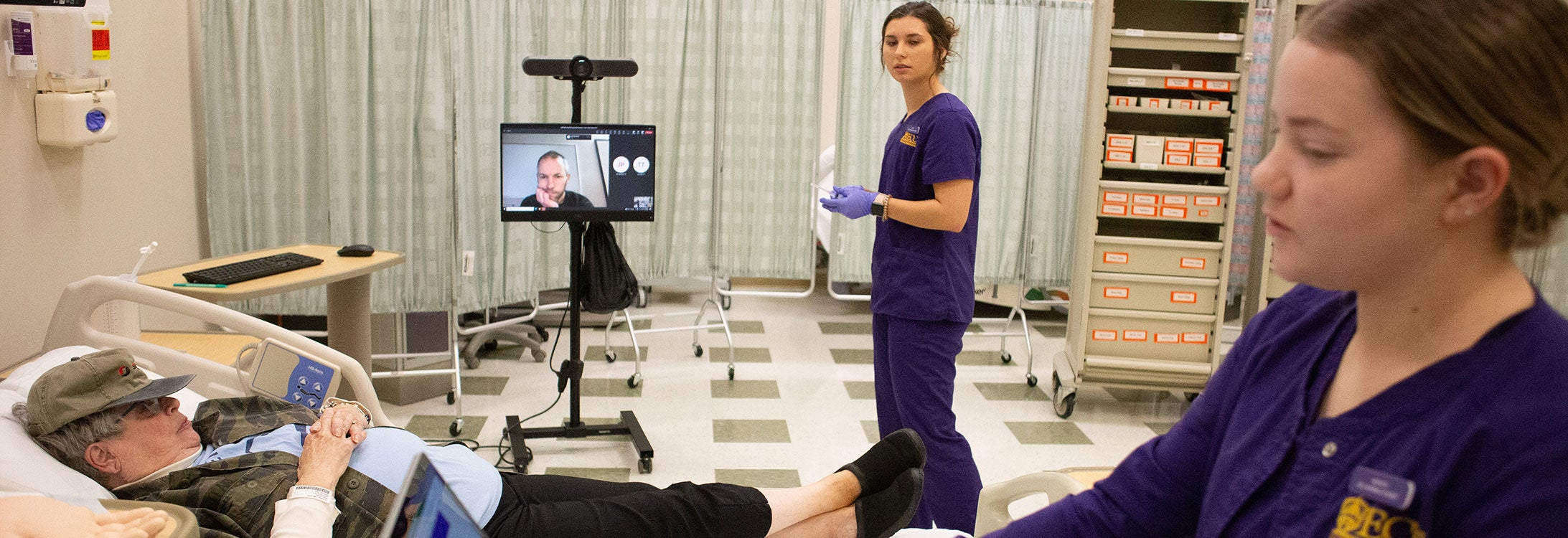
Nursing students partner though simulation to care for psychiatric patients
Dr. Tawny Tseng could never predict her path to becoming an East Carolina University nursing professor. A Seattle native, she was a jazz singer and then a dance teacher before joining the U.S. Air Force. While in uniform she repaired the electronic wiring on some of America’s most advanced, and secret, airplanes.
“I loved every second of it. I loved the smell of jet fuel. I was one of the first women on the flight line on my base. I think I was the first woman on many bases,” Tseng said.
Understanding how airplanes are wired, Tseng said, helped her understand how human neurology works, which has served her well as a psychiatric nurse and now a nursing professor.

Dominick Christou-Ader, an undergraduate nursing student, conducts a physical assessment with a standardized psychiatric patient during a simulation at the College of Nursing.
Tseng eventually moved to Hampstead, just north of Wilmington, with several small children and considered pursuing a law degree. As the primary caregiver she paid attention to the nurses who cared for her kids during routine office visits and was intrigued.
“I took my son to have some immunizations and he was terrified and screaming because of tactile sensitivity. The two nurses lured him to the back with his favorite candy, and they kept him back there until he calmed down so that I wouldn’t be distressed,” Tseng said. “They lied and told me that he did great — it was the greatest act of kindness I had ever seen.”
Tseng attended nursing school as soon as her family situation allowed. The care her kids received from nurses impressed her and she thought, “Maybe I could do that for somebody.” She started in emergency and trauma medicine, but it was working with psychiatric patients where she found her niche.
“How do you talk to people on the worst day of their life?” Tseng asked.
So, when Scott Eaves, a College of Nursing nurse consultant who manages the college’s simulation labs, proposed a simulation that would bring entry to practice nurses together with psychiatric mental health nurse practitioner (PMHNP) students – to learn from one another how to care for people having the worst day of their life – Tseng jumped at the chance.
The Idea
The idea seemed fairly simple: pair undergraduate nursing students with experienced nurses who are training to care for psychiatric patients to deal with a simulated emergency department intake assessment. But like many seemingly simple endeavors, this was layered with the complexity that nurses must be prepared to deal with before stepping into their roles after graduation.
Eaves said the undergraduate program historically offered behavioral health simulations, but there was no provider, or provider in training, for undergraduate students to consult with as would be the case in a real situation.
Eaves said there were some technical issues with having the PMHNP students piped in by computer to mimic a telehealth consultation, but those technical endeavors offered speedbumps that the simulation team was quick to overcome.
“You just deal with it on the fly, but it was a way of getting students together without making the PMHNP students commit a full day to come to campus — their schedules are busy, they are working, too,” Eaves said.
Undergraduate nursing students often have firsthand clinical experience with patients who are dealing with psychiatric difficulties, but usually only after they have emerged from an emergency phase of care and are better settled.
Dr. Adrian Lennon, another of ECU’s PMHNP faculty members who developed the simulation with Tseng, knows their students have likely cared for psychiatric patients, but not in the position of being the provider others are looking to for leadership and health care decision making.
“Our students are distance education anyway, so we got a chance to do simulation on telehealth in an emergency situation, which they may end up having to do on the job,” Tseng said of her PMHNP students.
Part of the impetus for the telehealth simulation is the challenged state of behavioral health care delivery in North Carolina. More than 40% of residents live in a mental health professional shortage area and less than half of North Carolinians who want to access mental health care are able to do so. Coverage in rural eastern counties is limited, especially for children and adolescents, for whom access to care is almost nonexistent.
Telehealth provides services where it physically isn’t, and where stigma prevents patients from seeking care.
“It’s prevalent in private practice,” Tseng said. “Telehealth has increased availability of psychiatric providers and decreased some of the stigma, because if I can see a provider virtually then I don’t have to worry about somebody seeing my car right outside of that provider’s office or running into them at the grocery store.”
Eaves noted that this simulation is adding opportunities for integrated training of health sciences students across the Health Sciences Campus.
“We’re keeping pace with what’s going on. Actually, we’re probably a little ahead of the curve. But the question is how do you do it, because everybody has different schedules,” Eaves said, noting a plan to have Brody School of Medicine fourth-year students conduct telehealth consultations for nursing students during a simulation this spring.
“Telehealth has really worked; I love it,” Tseng said. “If you struggle with therapeutic alliance, it can be a little more difficult on telehealth, but it is learnable. You can learn it, you really can, and that’s one of the reasons this was a really important part of the simulation.”
Eaves and College of Nursing instructors are extending the interprofessional education network — planning for near-term simulations that would extend to the social work program at the College of Health and Human Performance, as well as incorporating occupational and physical therapy students from the College of Allied Health Sciences.
Students Learning
Susan Lally, a PMHNP and College of Nursing clinical nursing instructor, lead the undergraduate aspect of the simulation that included consulting with a provider.

Nicole Dimino and Shayne Collins, undergraduate College of Nursing students, enter information into a simulated electronic health record during an emergency psychiatric patient assessment simulation.
“It was cool to watch them think things through, like ‘When do I call the provider? What information do I need to give them?’ and to struggle with trying to decide what the patient actually needs,” Lally said. “In school it’s hard for them to get that piece because they don’t interact with providers a whole lot. We teach in silos, so that piece might be missing when they end up in practice.”
Tseng said one of the most important parts of the learning experience for her PMHNP students was a demonstration of growing into their leadership role and showing empathy — to the simulated patient and to other students.
“It wasn’t ‘did you make the right diagnosis, did you pick the right medication?’ because that’s a learning process for them. This patient was not going to die, right?” Tseng said. “One of the most important parts of being a provider is being kind, not just kind to the patient, to everybody on the team and seeing it as a team and not a hierarchy.”
Lally said that after the simulation, the undergraduate students confided that being able to consult with providers, especially through the awkwardness of a telehealth scenario, helped erase some of the nervousness that they had going into the simulation.
“The first patient I had as a new nurse, like 16 years ago, was withdrawn and it was really scary. The fact that our students have already worked through it and practiced, they are going to feel more comfortable and know what to look for,” Lally said.
Tseng remembered that same feeling from her own undergraduate nursing education.
“I remember how terrified I was in simulation because you’re being watched by your peers, which is hard. You’re being watched by faculty,” Tseng said. “It shouldn’t feel hard because we love them so much.”
Translating the Classroom to the Bedside
Alexis Spence, a College of Nursing clinical nursing instructor who serves as the clinical coordinator for the college’s undergraduate mental health courses, works to place her students in hospitals and other setting where they can have firsthand experience with psychiatric patients. She values the simulations that she helped Eaves create, which allow her students a risk-free opportunity to think through the processes of providing emergency care.
“This is a very good way for them to bridge their medical-surgical skills and be able to look at severe and persistent mental illness along with substance abuse. This is one of those scenarios we don’t feel we can totally recreate in the clinical setting,” Spence said, because most psychiatric patients are in some form of treatment for acute symptoms before students see them in clinical rotations.
Spence believes that having her students equipped with the skills to work with psychiatric patients the first day on the job is critical.
“If they choose to work in an emergency department, a treatment center or a psychiatric unit, it’s very likely they will see patients in this condition,” Spence said.
Spence said she was very proud of how all the students responded to the scenario.
“I was pleasantly surprised at how good their therapeutic communication was. They had to use critical thinking skills and maintain safety, and they did a very good job,” Spence said.
Davina Ahlawat, a third semester nursing student from Raleigh, said that her clinical experiences thus far have given her less hands-on experience because their nurse preceptors in the hospital manage emergency patients before students interact with those patients at the bedside.
“It was new, and I really enjoyed it because that’s how it’s going to be in the hospital. In the clinical, emergency settings, the nurses have to handle it,” Ahlawat said.
Julie Webb, a third-semester student from Wilmington, said having a live person as a patient made the simulation even more realistic.
“We have communication back and forth with the patient instead of talking to a mannequin which made it a lot easier, but it also gives you more connection, to ask more questions, see what’s going on,” Webb said. “We able to formulate a plan and then execute the plan.”
Those plans were set askew by the live role players, though, which Webb valued.
“You don’t know what that patient’s going to do, if they’re going to walk out, if they’re going to have something in their pockets — anything could happen,” Webb said. “And you have to be aware of your surroundings, especially with a real person compared to a mannequin — they’re not going to walk anywhere.”